Uterine Fibroids: A Complete Overview
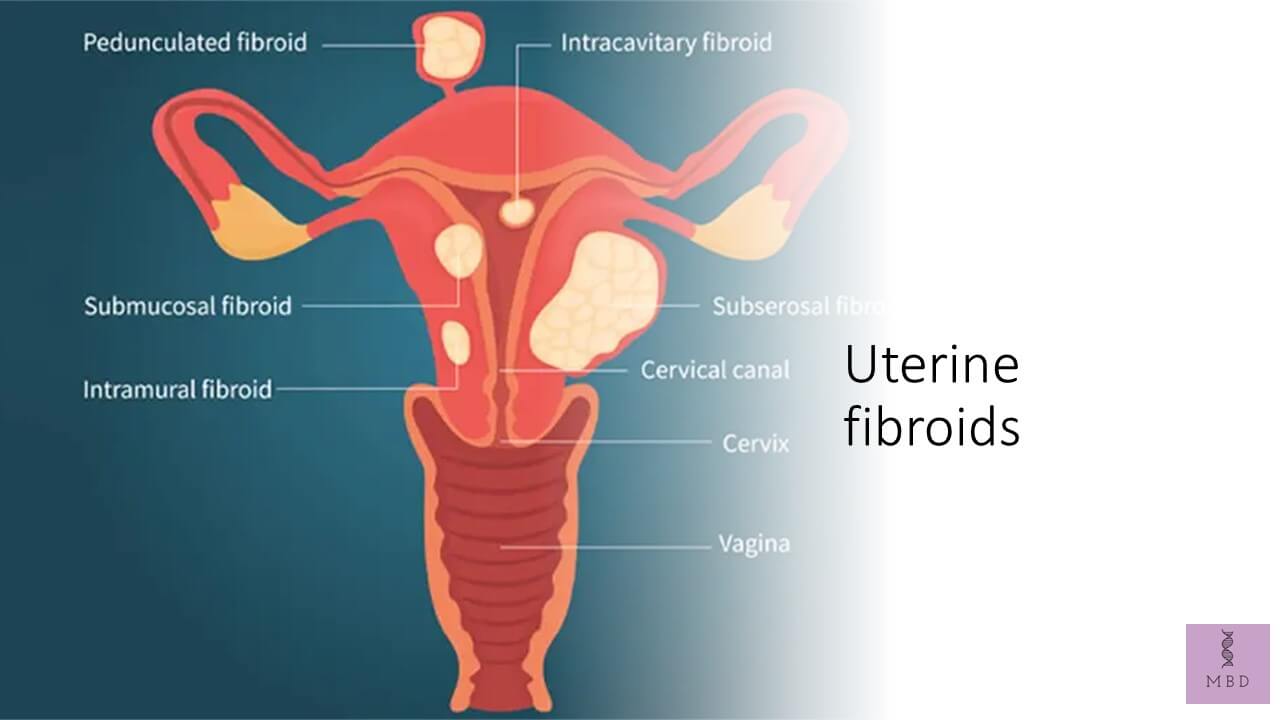
Common non-cancerous (benign) uterine tumours called uterine fibroids are the main justification for suggesting a hysterectomy. They are composed of muscle and fibrous tissue and develop from the uterus’s muscular wall. Fibroids are common in women over 35, however, they typically cause no symptoms.
A must read- What is a Mammogram? – My Biology Dictionary
Table of Contents
WHAT ARE FIBROIDS?
A fibroid is a benign growth (tumour) that primarily consists of fibrous tissue, such as muscle. Fibroids develop in or near the uterus (womb). They are the most typical form of growth in the pelvic region of women (the pelvis is the bony structure at the bottom of the spine).
UTERINE FIBROIDS
Noncancerous uterine growths known as uterine fibroids are common during the childbearing years. Uterine fibroids, also known as leiomyomas or myomas, don’t enhance the risk of uterine cancer and hardly ever turn into the disease.
Fibroids can be small enough to be invisible to the naked eye or large enough to stretch and expand the uterus. Fibroids can be isolated or spread out. In extreme circumstances, many fibroids may cause the uterus to enlarge to the point where it touches the rib cage and gains weight.
Around 30% of patients with uterine fibroids present symptoms and seek medical attention before the age of 50, according to estimates that 70% of women will have one or more uterine fibroids. Women of all ethnicities are affected, but those of African descent are more likely to develop fibroids and do so earlier in life. In comparison to Caucasian women of the same age, 60% of African-American women will have fibroids by the age of 35. Age (occurrence increases with age up to menopause, then often decreases in size), nulliparity, hereditary factors, early menarche, coffee, alcohol, obesity, and hypertension are additional risk factors.
CAUSES OF UTERINE FIBROIDS
Genetic alterations– Numerous fibroids have gene alterations that are distinct from those found in ordinary uterine muscle cells.
Hormones– The two hormones oestrogen and progesterone, which encourage the uterine lining to form during each menstrual cycle in preparation for pregnancy, also appear to encourage the growth of fibroids.
Compared to regular uterine muscle cells, fibroids have a higher concentration of oestrogen and progesterone receptors. As hormone production declines after menopause, fibroids frequently get smaller.
Additional growth factors– The development of fibroid tumours may be impacted by substances that aid in tissue maintenance, such as insulin-like growth factors.
Extracellular matrix (ECM)- ECM is the substance that binds cells together, just like mortar holds bricks together. Increased ECM makes fibroids more fibrous. Additionally, the ECM stores growth substances and modifies the biology of the cells.
SYMPTOMS
Most women do not have symptoms of fibroids. At least 25% of women with uterine fibroids experience symptoms, which can range from heavy bleeding or painful periods to bleeding between periods, cramping, bloating in the lower belly (abdomen or pelvic area), feeling full during sex, low back discomfort, and frequent urination.
Additionally, fibroids may result in infertility (the inability to become pregnant), miscarriages, or early labour (labour before 37 weeks of pregnancy).
HOW CAN UTERINE FIBROIDS BE DIAGNOSED?
During a normal pelvic exam, fibroids may be detected for the first time. Several tests could reveal further details regarding fibroids:
- An ultrasound examination makes an image of the uterus and other pelvic organs using sound waves.
- A narrow instrument called a hysteroscope is used in hysteroscopy to view the uterus’ inside. Through the cervix and vagina, it is inserted (opening of the uterus). This enables your medical practitioner to see uterine fibroid growth.
- A specialised X-ray test is a hysterosalpingography. The uterus and fallopian tubes may show abnormal changes in size and shape.
- A procedure called a sonohysterogram involves injecting fluid via the cervix into the uterus. After that, ultrasound is utilised to reveal the uterus’ inside. The fluid gives an accurate representation of the uterine lining.
- A narrow instrument called a laparoscope is used during laparoscopy to allow your doctor to see into your abdomen. It is implanted via or just below the belly button through a little incision. The laparoscope can be used to see fibroids that are external to the uterus.
Although they are not always necessary, imaging tests like computed tomography (CT) and magnetic resonance imaging (MRI) scans may be utilised. These tests could be useful in some cases to monitor the development of fibroids over time.

Image source: www.ultrasoundcases.info
RISK FACTORS INVOLVED IN UTERINE FIBROIDS
The following elements may influence a woman’s likelihood of developing uterine fibroids: 2,3:
- African American race; age (older women are more at risk than younger women);
- Soybean milk use;
- Obesity;
- Family history of uterine fibroids;
- High blood pressure;
- No prior experience with pregnancy;
- Vitamin D insufficiency
RELATION OF UTERINE FIBROIDS WITH CANCER
Cancer and fibroids don’t directly cause or result in one another. It’s possible that the same genetic or lifestyle variables that put you at risk for fibroids also put you at risk for uterine cancer.
But with the right medical attention and a healthy lifestyle, you can manage numerous risk factors. A healthy diet and regular exercise can reduce your risk of developing cancer. Additionally, routine checkups and screenings assist in detecting cancer while it is still curable.
TREATMENT
Medications
Ibuprofen or acetaminophen are examples of over-the-counter drugs that can be used to treat mild to moderate pain or discomfort on occasion. If taken during the first trimester of pregnancy, over-the-counter NSAIDs like ibuprofen may result in miscarriage.
Using Hormones
Oral contraceptives, often known as birth control tablets, can be used to manage fibroids’ bleeding symptoms. Low-dose birth control tablets or progesterone-similar injections (like Depo-Provera) do not promote the growth of fibroids and can be used to manage severe bleeding.
Surgery
For fibroids, three surgical procedures are available:
1. Myomectomy involves removing uterine fibroids
2. Endometrial Ablation involves damaging or removing the uterine lining, and
3. Hysterectomy involves removing the entire uterus.
Also check out- Azithromycin: Uses, Dosage and Side effects – My Biology Dictionary
Embolization
A nonsurgical technique called uterine artery embolization (UAE) or uterine fibroids embolization (UFE) stops the blood supply to uterine fibroids. Embolization is carried out under local anaesthetic without the need for skin incisions or cuts. The blood vessels that supply the fibroid with blood are inserted with a small, flexible tube, and a solution is then administered. This causes the fibroid to contract by cutting off its blood supply. Embolization causes fibroids to shrink by at least 50%. Because it is supplied by other arteries, healthy uterine tissue typically does not suffer any damage.
Summary
Uterine fibroids, also known as leiomyomas or myomas, don’t enhance the risk of uterine cancer and hardly ever turn into the disease. They are composed of muscle and fibrous tissue and develop from the uterus’s muscular wall. Fibroids are common in women over 35, however, they typically cause no symptoms. At least 25% of women with uterine fibroids experience symptoms, which can range from heavy bleeding or painful periods to cramping and bloating. Fibroids may result in infertility (the inability to become pregnant) or miscarriages, or early labour (labour before 37 weeks of pregnancy). Myomectomy involves removing uterine fibroids. One should be aware of the symptoms of Uterine Fibroids and take precautions actions.
Thanks for reading!
Team MBD
Reference:
- Uterine fibroids – what’s new? – PMC (nih.gov)– Williams, A. R. (2017). Uterine fibroids–what’s new?. F1000Research, 6.


